Who is the intensivist?
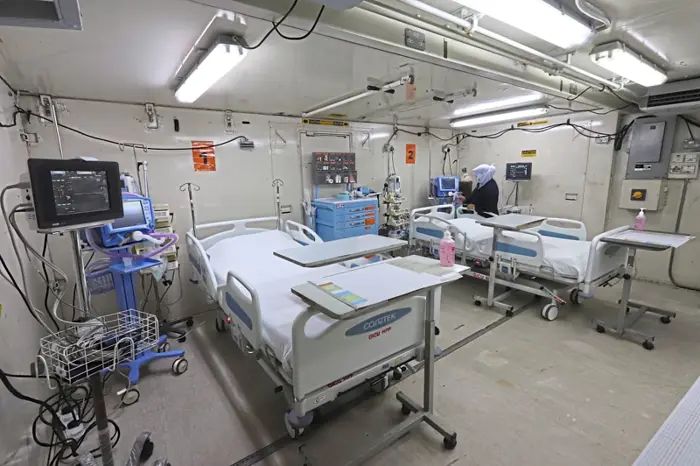
A staff nurse preps the field hospital ICU set up by the Armed Forces at Kepala Batas Hospital in Penang during the Covid-19 pandemic. ICUs require both the right equipment and enough staff to function well. — Filepic
Intensivists are specialised physicians who manage critically ill patients in intensive care units (ICUs).
These medical professionals must have completed an accredited intensive care training programme and possess advanced certification, ensuring their expertise in critical care medicine.
Primarily stationed within critical care units, intensivists are responsible for overseeing and directing complex treatment regimens for patients experiencing severe health crises.
A recognised subspeciality
The inception of ICUs in Malaysia dates to the 1960s, with University Hospital (now known as Universiti Malaya Medical Centre), pioneering the establishment of a fully operational ICU in Kuala Lumpur.
This innovative development rapidly spread throughout the country, leading to the widespread presence of ICUs in state hospitals by the mid-1990s.
These units were managed by anaesthesiologists, with support from surgeons and physicians.
As intensive care medicine evolved as a distinct medical subspeciality, an increasing number of anaesthesiologists – and subsequently, internal medicine physicians – undertook additional training to focus their practice in this subspeciality.
This was in line with the growing global trend of specialists identifying primarily as intensive care specialists, known as intensivists.
In 2009, the National Specialist Register formally established criteria for clinicians to be registered as intensivists, marking the official recognition of the term and of intensive care as a subspeciality.
Concurrently, it explicitly acknowledged the continuing significant role of anaesthesiologists in ICU management nationwide through the designation of the anaesthesiology speciality in the National Specialist Register as “Anaesthesiology and Critical Care”.
What’s in the ICU?
The standard of ICUs in Malaysia is high, especially in urban centres and government tertiary hospitals.
The Health Ministry sets strict guidelines for ICU operation and accreditation.
ICUs generally have controlled access, whereby entry is restricted and there are keycard/intercom systems to minimise infection risk and disturbance.
Most modern ICUs use an open bay concept with partial walls or curtains for easy visibility, though newer units are increasingly incorporating single isolation rooms for infectious patients (e.g. those with Covid-19 or the superbug methicillin-resistant Staphylococcus aureus [MRSA]) or those requiring extreme privacy.
There is a central nursing station at a strategic location to provide an unobstructed view of all patients.
It is the hub for monitoring and documentation.
Most ICUs have negative-pressure isolation rooms, which are essential for containing airborne pathogens.
These are a standard feature in most public and private hospital ICUs.
Environmental control is aided by advanced air filtration systems (HEPA filters), as well as controlled temperature and humidity to prevent infections.
There is adequate lighting, which is usually a combination of bright clinical lights for procedures, and softer, adjustable lights to help maintain patients’ circadian rhythms.
Each bed space has an “ICU pendant” or column that provides medical gases (oxygen, compressed air, vacuum/suction), multiple electrical outlets (often with backup power), and data ports for monitors and devices.
At the core of ICU support is the advanced monitoring and life-support equipment used to continuously display real-time data.
Among the pivotal life-support equipment that is part of the ICU armamentarium are mechanical ventilators, continuous renal replacement therapy machines, portable ultrasound machines, and other emergency equipment used to manage airway and circulatory collapse.
Who’s in the ICU?
Staffing in the ICU mainly comprises the nursing team and the allied healthcare team, which is made up of physiotherapists, pharmacists and dietitians.
Nurses are the backbone of the ICU.
The nurse-to-patient ratio is crucial.
It is typically 1:1 for the most critical patients and 1:2 for more stable ones.
ICU nurses are highly trained in critical care.
Pharmacists who work in the ICU are specialised in critical care pharmacology, advising on complex drug interactions and dosing.
Physiotherapists are vital for chest physiotherapy to clear secretions, and for early mobilisation and rehabilitation of patients.
Dietitians, on the other hand, calculate nutritional requirements and recommend feeding plans (enteral or parenteral nutrition).
At the helm of all this is the intensivist, who is akin to the conductor of an orchestra, using the baton to wield each and every piece of equipment and personnel for the best coordinated care of the patient.
The ‘conductor’s’ job
The daily routine of an intensivist is multifaceted, beginning with a morning handover where updates from the post-night team regarding existing patients and new admissions are discussed.
This is followed by morning rounds, which constitute the most critical and demanding segment of the day, involving a comprehensive review of each case.
This includes conducting thorough examinations, reviewing medications and ordering necessary investigations or imaging.
During this time, multidisciplinary team meetings and family conferences are held, ensuring that patients’ families are regularly updated, especially in cases of rapid or unexpected deterioration.
Coordination with multidisciplinary teams is imperative, with allied health teams such as pharmacists, respiratory therapists and dietary physicians contributing their expertise to the patient’s holistic care.
A significant portion of the day is dedicated to performing critical procedures such as intubations, central line insertions and managing dialysis.
These hands-on tasks require precision and swift decision-making, underscoring the intensivist’s central role in critical care.
Regular assessment of patient conditions is necessary, with intensivists dynamically adjusting treatments in response to evolving clinical scenarios.
Afternoon rounds provide another opportunity to review patient progress, address any emergent issues and ensure continuity of care.
Intensivists may also conduct training sessions for junior doctors, fostering an environment of continuous learning and professional development.
Undoubtedly, one of the defining roles of an intensivist is decision-making.
They must decide on the best possible treatment plan for critically ill patients, who often have fragile health and a high risk of death, making timely intervention crucial.
They also face the challenge of prioritising admissions to the unit, particularly when multiple patients require urgent care amid significant bed and staff constraints.
Amid all this, intensivists often find themselves navigating complex ethical dilemmas.
Decisions around end-of-life care, withdrawal of support and organ donation are profound aspects of the role, demanding a compassionate, yet pragmatic approach.
These situations require a delicate balance between medical intervention and respecting patient autonomy.
Family involvement is another cornerstone of intensive care, with intensivists often acting as mediators to communicate complex medical information, prognosis and potential outcomes.
These interactions are handled with sensitivity and empathy, aiming to align treatment goals with patient and family expectations.
In addition to their daily responsibilities, intensivists play a pivotal role in significant initiatives such as the intensive care registry and professional societies.
The Malaysian Registry of Intensive Care (MRIC), established in 2002, helps assess key progress indicators of ICUs and aids in quality improvement for intensive care services nationwide.
The Malaysian Society of Intensive Care (MSIC), which was established in 2009, provides a platform for intensive care specialists to collaborate locally and internationally.
The society focuses on education, clinical guidelines, scientific meetings and research grants to advance critical care.
The role of the intensivist is both physically and emotionally demanding.
Intensivists frequently undertake extended shifts with minimal rest, operating in high-pressure environments that require sustained attention and adaptability.
International standards recommend an intensivist-to-patient ratio between 1:8 and 1:15.
However, in hospitals under the Health Ministry, the ratio stands at approximately 1:13 to 1:30.
The emotional toll of the job is significant, as intensivists often form strong bonds with patients and their families during difficult times.
Witnessing the recovery of patients can be incredibly rewarding, yet the loss of a patient may equally be devastating.
It is not uncommon for intensivists to experience burnout, given the high stakes and relentless nature of their work.
In conclusion, the life of an intensivist is marked by a blend of technical expertise, emotional resilience and uncompromising dedication.
Their work is foundational to the functioning of ICUs, providing critical support to patients who are at their most vulnerable.
Through meticulous care, ethical integrity and a commitment to education and research, intensivists make an indelible impact in the field of healthcare.
Dr Gaithridevi V. Singam is an anaesthesiologist and intensivist. This article is the first in a three-part series on intensive care that will be published weekly, and is courtesy of the MSIC. For more information, email [email protected]. The information provided is for educational and communication purposes only, and should not be considered as medical advice. The Star does not give any warranty on accuracy, completeness, functionality, usefulness or other assurances as to the content appearing in this article. The Star disclaims all responsibility for any losses, damage to property or personal injury suffered directly or indirectly from reliance on such information.
← Back

